Severe Maternal Morbidity and Mortality in the United States (updated 8/2/24)
- Jeanette Zocco
- Jun 26, 2024
- 8 min read
Updated: Mar 7, 2025

Sanari’s story
Two days after the birth of her second child, Sanari began to feel significant abdominal pain that continued to worsen. She described not feeling right but was assured by the nurses that this was just gas. Despite the assurance, she knew this was not normal. She was taking pain medications including narcotics, suppositories, and Gas-X with continued break-through pain and subsequent development of odorous discharge. A different hospital diagnosed her with an 11-centimeter abscess on her uterus, and she was very close to developing sepsis. “I'm glad I didn't stop at no and I'm glad someone finally heard me, someone finally listened to me and, you know, didn't just take the generic, it's just gas, answer” (Centers for Disease Control and Prevention, 2024, para. 7).
Sanari’s narrative is unfortunately one of many in the Centers for Disease Controls (CDC) Hear Her Campaign, which details story after story of women who have experienced significant pregnancy-related complications. Pregnancy is often associated with young, healthy patients and good outcomes. Yet, the literature over the past 2 decades has consistently demonstrated a rise in severe complications and death during pregnancy and the postpartum period. This article discusses severe maternal morbidity and mortality in the United States, delving into the data, racial and ethnic disparities as contributing factors, major causes, and suggested solutions.
Definition and measurement of severe maternal morbidity
There is no standard definition or measurement for severe maternal morbidity (SMM).
SMM has been described as the “unintended outcomes of the process of labor and delivery that result in significant short-term or long-term consequences to a woman’s health” (ACOG, 2021,para 2). It has markedly increased in the United States, is highly preventability, and worthy of equal attention. SMM can be viewed as a near miss metric for maternal mortality, as some cases could have led to maternal death without appropriate recognition and treatment (ACOG, 2021).
Two common methods to identify women with SMM include using an index developed by the CDC and birth certificate information. The CDC identifies SMM by using healthcare administrative data based on diagnostic and procedure codes that reflect pregnancy associated conditions and procedures. Specifically, this is hospital discharge data in combination with specific procedure and International Classification of Diseases (ICD) diagnosis codes (CDC, 2024). Table 1 below contains the list used by the CDC. It is important to note that using this data for case identification is dependent on correct coding. Patient cases may be missed if not appropriately coded.
Table 1: SMM Indicators Used by the CDC
Acute Myocardial Infarction
| Conversion of Cardiac Rhythm | Severe Anesthesia Complications |
Aneurysm | Disseminated Intravascular Coagulation | Sepsis |
Acute Renal Failure | Eclampsia | Shock
|
Amniotic Fluid Embolism | Heart Failure / Arrest During Surgery or Procedure | Sickle Cell Disease with Crisis
|
Acute Respiratory Distress Syndrome | Puerperal Cerebrovascular Disorders | Air and Thrombotic Embolism
|
Cardiac Arrest / Ventricular Fibrillation | Pulmonary Edema / Acute Heart Failure | Hysterectomy
|
Temporary Tracheostomy | Ventilation | Blood transfusion * |
(Centers for Disease Control and Prevention, 2024)
*Excluded, but may be evaluated separately
Birth certificate data is also used due to accessibility, using fields that are likely indicators of SMM such as blood transfusion, eclampsia, sepsis, and intensive care unit admission. This approach has not been shown to provide a robust source of data, with low sensitivity noted in capturing these conditions (Snowden et al, 2021). Variation in birth certificate completion has been noted among states, hospitals, and healthcare systems. In addition, this form may be completed by an attending provider, nurse, or administrative staff member. These all point to factors that may contribute to data discrepancies (Snowden et al, 2021).
Maternal mortality
There are three data sources that monitor maternal mortality on national and local levels. The Pregnancy Mortality Surveillance System (PMSS) and the National Vital Statistics System (NVSS) monitor from a national perspective. Maternal mortality review committees (MMRCs) monitor this information at state and local levels (CDC, 2024).
The PMSS monitors “deaths during pregnancy or within 1 year of the end of pregnancy from a cause related to pregnancy or its management” (Ahn et al, 2020, p. S3), and the NVSS monitors “deaths during pregnancy or within 42 days after the end of pregnancy from a cause related to pregnancy or its management” (Ahn et al, 2020, p. S3). Data from the PMSS has shown that complications in pregnancy resulting in death, impact approximately 700 women per year (Peterson et al., 2019). More recent NVSS data from 2018-2021 has shown a continued increase, from 17.4 to 32.9 deaths per 100,000 live births, with each year demonstrating a statistically significant increase from the prior year (Hoyert, 2023). (Figure 1).
Figure 1. Maternal mortality rates, by race and Hispanic origin: United States, 2018–2021

(Hoyert, 2023)
Racial and ethnic disparities
Figure 1 also speaks to racial and ethnic disparities - with non-Hispanic black mothers experiencing the highest mortality rates across all 4 years. In 2021, non-Hispanic Black women experienced mortality rates 2.6 times higher than non-Hispanic White women, with 69.9 and 26.6 deaths per 100,000 live births respectively. In addition, all race and Hispanic-origin groups experienced a statistically significant increase in maternal mortality from 2020 to 2021 (Hoyert, 2023). PMSS Mortality data from 2007 to 2016 also shows similar findings, with non-Hispanic Black women and American Indian/Alaska Native women experiencing a 3.2 and 2.3 times higher risk of death than their non-Hispanic White counterparts, respectively (Ahn et al., 2020).
Literature has shown racial and ethnic disparities are significant contributors to severe maternal morbidity as well, with studies showing women in every racial and ethnic minority classification have significantly higher delivery complications compared to non-Hispanic white women (Admon et al, 2018). Multiple sources are consistently showing a significant need to do better in maternal outcomes.
Causes of maternal mortality
Data from the PMSS has evaluated for causes of pregnancy-related death. The top causes from 2017-2019 include the following: other cardiovascular conditions, infection or sepsis, cardiomyopathy, hemorrhage, noncardiovascular medical conditions and thrombotic pulmonary or other embolism. See Figure 2 below for full details (CDC, 2023).
Figure 2: Causes of Pregnancy-related death in the United States: 2017-2019
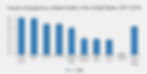
(CDC, 2023)
This is consistent with earlier PMSS data from 2011-2015, which showed cardiovascular conditions, infection, and hemorrhage as the leading causes of death (Peterson et al., 2019).
Maternal mortality review committees
State and local MMRCs provide valuable information to inform next steps by means of a thorough investigation into each patient death. This includes a review of multiple data sources such as medical, autopsy, and social service records. A standardized approach to data abstraction and multidisciplinary committee review is used. This information is used to understand the circumstances around each death, and determine if it was pregnancy-related and preventable. Information gathered from these committees is central to guiding solution development.
Data from 36 state MMRCs from 2017-2019 showed that over eighty percent of pregnancy-related deaths were preventable, with contributing factors identified in the following areas: community (transportation and housing difficulties), hospital-specific (inexperience managing obstetric emergencies and inadequate personnel or care services), patient (inadequate knowledge of maternal warning signs and nonadherence to medical plans), provider (failure or delay in diagnosis) and system-related (insufficient access to care and coordination of services) (Trost et al., 2022).
These contributing factors also reflect preventability around racial and ethnic disparities. For example, community factors include living situations that make it difficult to live a healthy lifestyle, such as few or limited healthy food alternatives, and inability to go outside and exercise due to high crime living areas. Variation in nurse staffing levels can create situations in which patients are not adequately monitored and critical vital sign changes can be missed. On a provider level, conscious and unconscious bias impacts decision making around care to women of color. This might look like disregarding patient complaints of pain or symptoms (Bingham, 2019). Sanari’s story earlier reflects this when her repeated complaints of pain were dismissed as gas instead of exploring further. Had she not sought treatment at another hospital, she could have become one of these statistics.
Lastly, Trost et al (2022) highlight two salient points:
53% of deaths occurred from 7 -365 days postpartum, a time in which most patients are home
Mental health conditions ranked highest (22.7%) as the most frequent underlying cause of pregnancy-related death. This includes suicide and overdose/poisoning associated with substance use disorder.
This was followed by hemorrhage, cardiac and coronary conditions, and infection, which is similar to previous reports.
Most recent data
The most recent data from the NVSS show a statistically significant decrease from 32.9 deaths per 100,000 live births in 2021 to a rate of 22.3 in 2022. This same trend is seen among Black non-Hispanic, White non-Hispanic, and Hispanic women (Figure 3) (Hoyert, 2024). Though this may seem promising, this reduction likely reflects a return to pre-pandemic levels.
Figure 3: Maternal mortality rate, by race and Hispanic origin: United States, 2021 and 2022

(Hoyert, 2024)
Severe maternal morbidity and mortality: next steps
A lot of work is underway to address these issues and there are many strategies to support the efforts. The following are a few examples of solutions to address the community-hospital-patient-provider and system factors:
Expand office hours and increase transportation access including vouchers for medical visits
Improve access to obstetric services in rural areas
Implement obstetric safety bundles including emergency protocols and training (ex. obstetric hemorrhage, severe hypertension, venous thromboembolism)
Implement obstetric early warning systems in hospitals to prompt early recognition and response
Implement a standardized process for screening and performing quality review for potential patient cases of SMM, using the following criteria:
(1) Patients who receive 4 or more units of blood
(2) ICU admission
This is supported by ACOG, SMFM, AWHONN, and ACNM (ACOG, 2021).
Improve patient education (office and hospital level) including maternal early warning signs (ex. AWHONN Save Your Life discharge instructions)
Improve communication between obstetricians and all support staff, including for hand-offs and critical events
Expand Medicaid coverage for up to 1 year postpartum (Peterson et al, 2019)
Stratify data to evaluate for racial and ethnic disparities
Offer implicit bias training to help raise awareness around unconscious assumptions that can drive care for women of color
*If this article interests you, you may also enjoy my book titled: Obstetric and Neonatal Quality and Safety (C-ONQS) Study Guide: A Practical Resource for Perinatal Nurses, available on amazon: Amazon_obneonatalstudyguide
Copyright by Jeanette Zocco MSN, RNC-OB, C-EFM, C-ONQS
References
Ahn R., Gonzalez G., Anderson B., Manning L. (2020). Initiatives to Reduce Maternal Mortality and Severe Maternal Morbidity in the United States. Annals of Internal Medicine, 173(11), S3-S10. DOI:10.7326/M19-3258
American College of Obstetricians and Gynecologists (2021). Severe Maternal Morbidity: Screening and Review. Obstetric Care Consensus, Number 5.
Bingham D., Jones D., & Howell E. (2019). Quality Improvement Approach to Eliminate Disparities in Perinatal Morbidity and Mortality. Obstetrics and Gynecology Clinics of North America, 46, pp. 227–238. Retrieved June 10, 2024 from
Centers for Disease Control and Prevention. (2024, May 15). Hear Personal Stories of Pregnancy-Related Complications, Hear Her: Sanari’s Story. Retrieved June 8, 2024 from https://www.cdc.gov/hearher/personal-stories/videos/transcripts/Sanari-transcript-508.pdf
Centers for Disease Control. (2024, May 15). Identifying Severe Maternal Morbidity (SMM). Retrieved June 1, 2024 from https://www.cdc.gov/maternal-infant-health/php/severe-maternal-morbidity/icd.html
Centers for Disease Control. (2024, May 15). Pregnancy Mortality Surveillance System. Retrieved June 1, 2024 from: https://www.cdc.gov/maternal-mortality/php/pregnancy-mortality-surveillance/index.html
Centers for Disease Control. (2023, March 23). Reproductive Health. Pregnancy Mortality Surveillance System. Retrieved June 21, 2024 from file:///C:/Users/Jeanette%20Zocco/Downloads/cdc_128166_DS1.pdf
Hoyert D.L.(2023). Maternal mortality rates in the United States, 2021. NCHS Health E-Stats. DOI: https://dx.doi.org/10.15620/cdc:124678
Hoyert D.L.(2024). Maternal mortality rates in the United States, 2022. NCHS Health E-Stats. DOI: https://dx.doi.org/10.15620/cdc/152992
Admon, L.K., Winkelman, T., Zivin, K., Terplan, M., Mhyre, J.M., & Dalton, V.K. (2018) Racial and Ethnic Disparities in the Incidence of Severe Maternal Morbidity in the United States, 2012–2015. Obstetrics and Gynecology, 132 (5), pp. 1158-1166.
Peterson E., Davis N., Goodman D., Cox S., Mayes N., Johnston E., Syverson C., Seed K., Shapiro-Mendoza C., Callaghan W., & Barfield W. (2019). Vital Signs: Pregnancy-Related Deaths, United States, 2011-2015, and Strategies for Prevention, 13 States, 2013-2017. Morbidity and Mortality Weekly Report, 68(18), pp. 423-429.
Snowden J., Lyndon A., Kan P., El Ayadi A., Main E., & Carmichael S. (2021). Severe Maternal Morbidity: A Comparison of Definitions and Data Sources. American Journal of Epidemiology, 190(9), pp.1890–1897, Retrieved May 20, 2024 from https://doi.org/10.1093/aje/kwab077.
Trost S., Beauregard J., Chandra, G., Njie F., Berry, J., Harvey, A., & Goodman, D. (2022). Pregnancy-Related Deaths: Data from Maternal Mortality Review Committees in 36 US States, 2017–2019. Atlanta, GA: Centers for Disease Control and Prevention, US Department of Health and Human Services
Disclaimer:
The use of the CDC data figures and reference links does not imply endorsement by CDC, ATSDR, HHS or the United States Government of Perinatal Quality and Safety Resources LLC or Obneonatalstudyguide.com. The CDC cited material is otherwise available on the agency website for no charge.
